Estimated reading time: 4 minutes
Psoriatic arthritis is a type of arthritic inflammation that occurs in about 15 percent of patients who have a skin rash called psoriasis. This particular arthritis can affect any joint in the body, and symptoms vary from person to person. Research has shown that persistent inflammation from psoriatic arthritis can lead to joint damage. Fortunately, available treatments are effective for most people.
Table of contents
Fast Facts
- Diagnosis is important to avoid damage
- Psoriatic arthritis can occur in people without skin psoriasis, particularly in those who have relatives with
- Physical activity helps maintain joint
Psoriatic Arthritis in Dubai, UAE?
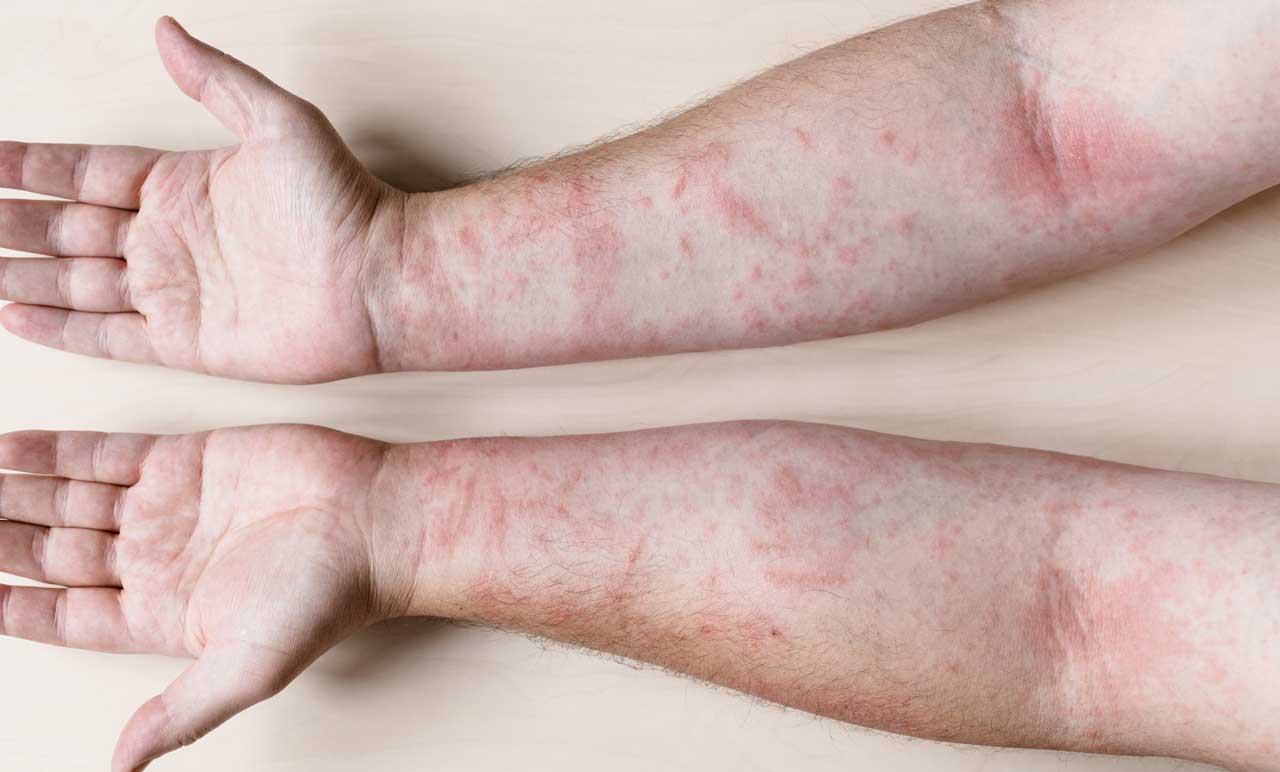
Psoriasis is a disease in which scaly red and white patches develop on the skin. Those with psoriasis can also develop psoriatic arthritis when the body’s immune system goes into overdrive to attack the skin disease, causing inflammation in the joints. Like psoriasis, psoriatic arthritis symptoms flare and subside, vary from person to person, and even change locations in the same person over time.
Psoriatic arthritis in Dubai, UAE can affect any joint in the body, either in a single joint or in the same joint on both sides of the body. For example, it may affect one or both knees. Affected fingers and toes can resemble swollen sausages, a condition often referred to as dactylitis. Finger and toe nails also may be affected.
Psoriaticarthritisinthespine, called spondylitis causes pain in the back or neck, and difficulty bending. Psoriatic arthritis also can cause tender spots where tendons and ligaments join onto bones. This condition, called enthesitis, can result in pain at the back of the heel, the sole of the foot, around the elbows or in other areas. Enthesitis is one of the characteristic features of psoriatic arthritis. Recent research suggests that persistent inflammation from psoriatic arthritis causes joint damage later, so diagnosis is essential. Fortunately, treatments are available and effective for most people.
What Causes Psoriatic Arthritis in Dubai, UAE?
What causes psoriatic arthritis is not known exactly. Of those with psoriatic arthritis, 40 percent have a family member with psoriasis or arthritis, suggesting heredity may play a role.
Psoriatic arthritis can also result from an infection that activates the immune system. While psoriasis itself is not infectious, it might be triggered by a streptococcal throat infection.
Who Gets Psoriatic Arthritis?
Psoriatic arthritis usually appears in people between the ages of 30 to 50, but can begin as early as childhood. Men and women are equally at risk.
Approximately 15 percent of people with psoriasis develop psoriatic arthritis. At times, arthritis can appear before the skin disorder.
Psoriatic arthritis typically affects the large joints, especially those of the lower extremities, distal joints of the fingers and toes, and can also affect the back and sacroiliac joints of the pelvis.
How Is Psoriatic Arthritis Diagnosed?
To diagnose psoriatic arthritis, rheumatologists look for swollen and painful joints, certain patterns of arthritis, and skin and nail changes typical of psoriasis. X-rays often are taken to look for joint damage. MRI or CT scans also can be used to look at the joints in more detail.
Occasionally skin biopsies (small samples of skin removed for analysis) and blood tests are done to rule out other types of arthritis that have similar signs and symptoms, including gout and rheumatoid arthritis. In patients with psoriatic arthritis, blood tests may reveal high levels of inflammation and mild anemia.
How Is Psoriatic Arthritis Treated?
Treatment varies depending on the level of pain. Those with very mild arthritis may require treatment only when their joints are painful and may stop therapy when they feel better.
Non-steroidal anti-inflammatory drugs such as ibuprofen (Motrin or Advil) or naproxen (Aleve) are used as initial treatment. If arthritis does not respond, disease-modifying anti-rheumatic drugs may be prescribed. These include sulfasalazine (Azulfidine), methotrexate (Rheumatrex), cyclosporine (Neoral, Sandimmune), leflunomide (Arava) and the more recently available “anti-TNF agents” such as etanercept (Enbrel), infliximab (Remicade) and adalimumab (Humira). The anti-malarial drug hydroxychloroquine (Plaquenil) may help, but it usually is avoided as it can cause a flare of psoriasis.
Azathioprine (Imuran) may help those with severe forms of psoriatic arthritis. For severely swollen joints, corticosteroid injections can be useful. Surgery can be helpful to repair or replace badly damaged joints.
Living With Psoriatic Arthritis
Many people with arthritis develop stiff joints and muscle weakness due to lack of use, so proper exercise is very important, as it will improve overall health and keep joints flexible.
Walking is an excellent way to get exercise. A walking aid or shoe inserts will help to avoid undue stress on feet, ankles, or knees affected by arthritis. An exercise bike provides another good option, as well as yoga and stretching exercises to help with relaxation.
Some people with arthritis find it easier to move in water. If this is the case, swimming or walking laps in the pool offers activity without stressing joints.
Many people with psoriatic arthritis also benefit from physical and occupational therapy to strengthen muscles, protect joints from further damage, and increase flexibility.
POINTS TO REMEMBER
- Psoriatic arthritis is chronic In some people, it is mild, with just occasional flare-ups. In other people, it is continuous and can cause joint damage if it is not treated.
- For most people, appropriate treatments will relieve pain, protect the joints, and maintain
- Psoriatic arthritis is sometimes misdiagnosed as or can be associated with other conditions,